As a neurology resident in the late 1990s, David Newman-Toker, MD, PhD, saw multiple patients leave the emergency department (ED) with undiagnosed neurological conditions, only to return with serious complications like blindness and paralysis. Among the most common culprits was dizziness, a potentially deceptive symptom that usually indicates a self-limited inner-ear disorder — but can sometimes result from a stroke.

By the time Newman-Toker came to Johns Hopkins in 2000 to do a clinical fellowship in vestibular neurology under David Zee, MD, he was already searching for ways to help doctors in the ED distinguish serious causes of dizziness from benign ones. Now, as the inaugural recipient of the David Robinson Professorship in Vestibular Neurology, Newman-Toker, who took over from Zee as director of the Division of Neuro-Visual and Vestibular Disorders in 2015, is closer than ever to achieving his goal.
Newman-Toker intends to use the research-focused professorship to drive the development of a tiered, tech-driven system to more effectively manage dizzy patients. The late Hopkins neuroscientist and biomedical engineer David Robinson made the initial endowment gift through his estate, which was followed by contributions from colleagues of his, grateful patients who received care in the vestibular clinic, and the Maryland E-Nnovation Initiative — a state-financed program supporting basic and applied research at colleges and universities that will spur economic development, and which is providing $1.8 million in matching funds.
Dizziness represents a significant public health problem. According to Newman-Toker, who holds a doctorate from the Johns Hopkins Bloomberg School of Public Health, 18 million Americans seek medical care for dizziness each year, 5 million of them through the ED. Most of those dizzy patients suffer from nonthreatening conditions like vestibular neuritis, caused by inflammation of the so-called balance nerve, which connects the inner ear and brain. But the vestibular system that helps us maintain our balance involves a complex ballet between our ears, eyes, and brains. If any part of that system is disrupted, dizziness or vertigo can ensue; and sometimes the cause is a stroke inside the brain itself.
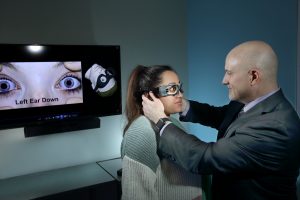
Vestibular neurologists like Newman-Toker and Zee can diagnose the underlying cause by carefully examining a patient’s eye movements, since subtle abnormalities in how we track objects and fix our gaze indicate lesions in particular parts of the brain. In 2009, for example, Newman-Toker and colleagues published a study proving that a series of bedside eye-movement tests sorted strokes from inner-ear disorders more accurately than brain MRIs, which were previously the best available test.
Unfortunately, many frontline physicians are unfamiliar with those tests, which require time and training to master; and there simply aren’t enough properly trained specialists to go around. As a result, says Newman-Toker, nearly 40% of strokes manifesting dizziness or vertigo go undiagnosed, often with devastating consequences.
“Dizzy strokes are often an early warning shot,” Newman-Toker says. “You either get lucky and don’t have a major stroke after that warning shot, or you get unlucky and have a devastating stroke that is permanently disabling or even lethal. But if we recognize the manifestations of a dizzy stroke immediately, we can usually prevent the major one.”
Now Newman-Toker is poised to solve the problem of undiagnosed dizzy strokes by using technology to democratize access to expert diagnostic knowledge.
Working closely with colleagues at Hopkins and elsewhere, Newman-Toker has developed innovative ways to use high-tech video goggles that can accurately record a dizzy patient’s eye and head movements. The data collected by these “stroke goggles” can then be interpreted remotely by a specialist. (The goggles are being used to remotely diagnose strokes in patients at the Johns Hopkins Hospital through a clinical program called Tele-Dizzy that is currently expanding to other EDs in the Johns Hopkins Health System). Newman-Toker and his team are also building software algorithms to help non-specialists diagnose strokes as well. And they are developing an app called “eyePhone” that uses similar algorithms to analyze video taken with a smartphone camera, allowing patients to receive an initial diagnosis at home.

In the future, people who wake up feeling dizzy might first use the eyePhone app to test their eye movements and answer a few basic questions: Can they self-treat at home, using only guidance from the app? Should they make an appointment to see their primary care physician? Or should they instead immediately dial 911 to call for an ambulance? Once at the clinic or the ED, a technician could have them don a pair of artificial-intelligence (AI)-enhanced video goggles for a more sophisticated algorithmic diagnosis. The toughest cases, meanwhile, would be referred to a vestibular specialist for remote diagnosis.
“We’re basically trying to find ways to more efficiently deliver expertise at scale,” says Newman-Toker, whose project builds upon a longstanding effort to improve clinical care through research and technology.
Robinson, who earned master’s and doctorate degrees in electrical engineering and a master’s in mathematics at Hopkins in the 1950s, was among the first to describe the neural circuitry that controls eye movements. In addition to developing a novel method for recording eye movements, Robinson correlated those movements with neural activity and developed mathematical models that allowed clinicians to relate specific eye movements to particular parts of the brain.

In 1972, Robinson met Zee, a graduate of the Johns Hopkins School of Medicine, and together they built a laboratory for investigating vestibular and eye-movement disorders in human subjects. Soon afterwards, Zee founded what is now known as the Division of Neuro-Visual and Vestibular Disorders; and he would go on to spend decades translating basic research into cutting-edge treatments for vestibular disorders while training scores of others — including Newman-Toker — to do the same.
“Dave’s goal was always to bring physiology, technology, and a rigorous analytical approach to the clinic,” Zee says of Robinson. “In a sense, Newman-Toker’s work is a culmination of this goal in the management of patients with stroke.”
But for Newman-Toker, the work has only just begun.
In the future, Newman-Toker hopes to use eye movements to diagnose other neurological conditions such as Alzheimer’s and Parkinson’s diseases. And he wants to use the blueprint he has drawn up for catching dizzy strokes (in-home screening, technologically enhanced emergency services, remote specialist care) to improve the diagnosis of everything from headaches to cancer.
“Dizziness,” he says, “is the tip of the spear.”
Interested in supporting life-changing research in vestibular and eye-movement disorders?
Topics: Faculty and Staff, Friends of Johns Hopkins Medicine, Johns Hopkins Medicine, Neurology, Fuel Discovery