Most surgical microscopes have names that sound like they’ve been pulled from the pages of a science fiction novel. The Lecia M530 OHX. The Zeiss OPMI 1. The Möller Spectra 500.
But in Amin Herati’s operating room, the floor-to-ceiling piece of cutting-edge equipment bears a plaque with a much more human name — Kara’s Microscope.
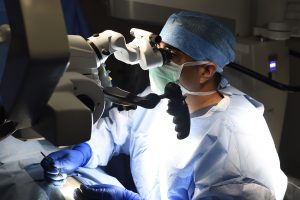
As the director of Male Infertility and Men’s Health and assistant professor of Urology at The James Buchanan Brady Urological Institute, Herati focuses on every aspect of men’s reproductive health, from hormones and sexual function to enlargement of the prostate. He specializes in male infertility, a condition he says is viewed very differently — and with much less recognition — than female infertility.
“It’s an intimate condition that guys and couples are dealing with. It’s not something that’s very easy for them to talk about, and being able to be in a position to help them is extremely important,” Herati says. “It’s a unique opportunity that they’re giving me, trusting in me to be in their lives and talk to them about an issue a lot of people don’t even know that they’re dealing with.”
Though Kara’s Microscope is already helping families, more funding is needed to support Herati’s research into the genetic basis of male infertility and the impacts of electromagnetic frequencies (EMF) — which can come from things like power lines and cell phones — on fertility.
Ten percent of couples globally encounter fertility problems, Herati says, and there’s little awareness of the issues that can lead to male infertility. Though female infertility interventions are far more common — workups are initiated on women 80% of the time — women and men are equally likely to experience the condition. In one third of cases, an isolated female infertility factor is identified. Similarly, a male factor is isolated one third of the time. The remaining cases encounter factors that are both male and female.
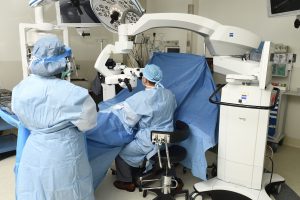
“In this field, we are taking care of patients. But we’re also spreading awareness that men need to be worked up because there are a lot of conditions that can lead to infertility that will have serious long-term repercussions for the health of the male if not identified,” Herati says. “Fifty percent of men who have no sperm in their ejaculate will also have low testosterone. There are things that we can identify early on before they develop other serious conditions.”
With Kara’s Microscope, Herati and his team are able to perform microsurgeries to help correct male infertility, including identifying, realigning, and reconstructing important structures in the male reproductive system. The operative microscope zooms in up to 20 times, allowing Herati to see submicroscopic structures and get as close as the inside of the vas deferens, the duct that carries sperm from the testicles to the urethra, which is about a hair follicle in thickness. With the microscope, Herati can put six sutures inside of the vas deferens, each about 0.2 millimeters thick.
The microscope also helps identify dilated tubules in men who have no sperm in their ejaculate. The difference in dilated and non-dilated tubules can be less than 200 micrometers — about the same thickness as a sheet of paper.
“We’re really trying to find minimally enlarged tubules to the naked eye, but when we use the microscope we can see them and identify them,” Herati says.
Of the 34 testicular sperm extractions Herati performed in the past 12 months, 31 led to microsurgeries, thanks to Kara’s microscope.
The microscope’s namesake, Kara, is Judy and Leo Zickler’s great-granddaughter. The Zicklers donated the equipment in recognition of Herati’s leadership role in helping their grandson and granddaughter-in-law after encountering initial hurdles with male infertility. Herati was able to extract sperm from Zickler’s grandson, which, combined later with in vitro fertilization, led to Kara and her sister, Brooklyn.
Now, Kara’s Microscope has helped dozens of families. Herati says the Zicklers’ support, and the support and trust of all his patients and their families, means everything.
“We have been supporting the research of The Brady for more than 25 years,” says Leo Zickler. “The leading-edge work of Dr. Herati has now given us the profound joy of adding two bundles of love to our family. We are now in our eighties — how much luckier can we get?”
Topics: Friends of Johns Hopkins Medicine, Johns Hopkins Medicine, The Brady Urological Institute, Fuel Discovery, Promote and Protect Health